Online Course
NDNP 810 - DNP Project Identification
Mod 3: Planning
Planning the Implementation
Identifying the Change
Making improvement requires making change. How do you know what to change and how to achieve change? To determine what to change, analyze the current process that you mapped and brainstorm with your team. Decide what is working and what could be done better.
- Are there steps in the current process that could be eliminated or combined? That would make practice more efficient. Review your process maps again.
- Should you reorder or add to the current process? That would make practice more effective.
- Consider the feasibility of making any changes and the interest or buy-in from the site to make that change. Think also about the decision-making authority to proceed and the responsibility for carrying out the change – do you have the resources?
Let’s say your organization has established a goal for patient discharges to occur in a timely manner, by 11:00 am each day. The purpose of this goal is to make beds/rooms available to accommodate new daily scheduled admissions.
- 20% of discharges on your unit take place by 11:00 a.m. each day
In response to the current underachievement of this goal, your unit mobilized a team to address the problem. The team identified a root cause of the problem as limited time between the desired discharge time (11:00 a.m. daily) and the time a provider enters a discharge order into the health record.
The team mapped the steps in the current discharge process and determined that most discharge orders are entered into the record following morning rounds, which begin around 7:00 a.m. daily. This results in a limited time interval between the desired discharge time (11:00 a.m. daily) and the time providers enter a discharge order into the health record.
The team hypothesized that the length of the interval between a desired patient discharge time and the time a provide enters a discharge order into the health record, would impact the timeliness of discharge. A review of the research showed that the longer the interval between the desired patient discharge time and the time a provide enters a discharge order into the health record, the more likely the patient was to be discharged in a timely manner.
At this point, your team has identified a(n):
- Problem
- Root cause
- Current Process
- Desired Process
- Goals
- Evidence-based solution
- Framework
Planning the Change
The team's first task when planning is to establish an aim or goal for the improvement work. By setting this goal, you will be better able to clearly communicate your objectives to all the sectors in your organization that you might need to support or help implement the intervention. The goal should reflect the specific aspects of the performance that the team is targeting and should be measurable and achievable.
Based on the research evidence, the team identified the following goal:
- 100% of all patients will have a discharge order entered into the record 12 hours in advance of the target discharge time.
Let’s use the Conceptual Framework of Complex Innovation Implementation to plan our change. This Framework demonstrates that implementation effectiveness is achieved as the result of management support, availability of resources, use of policies and procedures, change champions, and organizational values and climate:
- do you have management support and resources to implement the project?
- are there written policies and procedures in place?
- do you have change champions on your team who support the initiative?
- Is the organizational climate supportive and receptive to change?
- If not, your implementation plan will involve strategies and tactics to address any component that is absent or lacking.
Implementation Strategies and Tactics
Strategies and tactics are specific actions that are expected to achieve a certain goal or aim. Implementation leaders will be more effective if their implementation plan includes multiple types of strategies and tactics. Too often leaders’ default to only one strategy, education. Education is the first stage when disseminating an innovation. However, leaders need to utilize other strategies and tactics as well. Since implementation is context specific, there is no one list of strategies and tactics that apply to every initiative.
Be creative and identify strategies and tactics that are considered a good fit for your organization and the goals you’re trying to achieve. The success of your DNP Project depends on how willing people are to work with you. You do not have the ability to dictate that others change. You can however lead in a manner that influences, persuades, and supports others in their efforts to improve outcomes.
Consider the ABCDE acronym below to guide the identification of possible strategies and tactics for your DNP project (Bingham & Main, 2010; Powell et al., 2015). Refer to this link for a detailed list of suggested implementation strategies and tactics
A = Accountability
B = Buy-In for the right outcomes
C = Collaboration, Communication, and Changes in structures
D = Data
E = Education
Barriers and Facilitators
The team will need to consider the psychological, physical, and procedural barriers it has to address in order to accomplish its aim. Barriers to improvement come in many forms. Psychological barriers such as fear of change, fear of failure, grief over loss of familiar processes, or fear of loss of control or power can be significant impediments to overcome. Other common barriers include the following:
- Inexperience with quality improvement, lack of support or buy-in
- Deficient knowledge or ability, lack of training
- Inadequate staffing levels and/or resources.
- Limited information technology systems.
- Outdated or misguided organizational policies.
QI Data Analytics
Quality Improvement looks to show that strategies and tactics worked to bring about measurable change. This change is measured by tracking data over time, commonly referred to as time series analysis. Change from pre-intervention throughout an intervention phase, best illustrated by run chart. The basic anatomy of a run chart includes time on the x-axis (for our purposes weeks) and process or outcome values on the y-axis. Individual data points are plotted in the body of the chart.
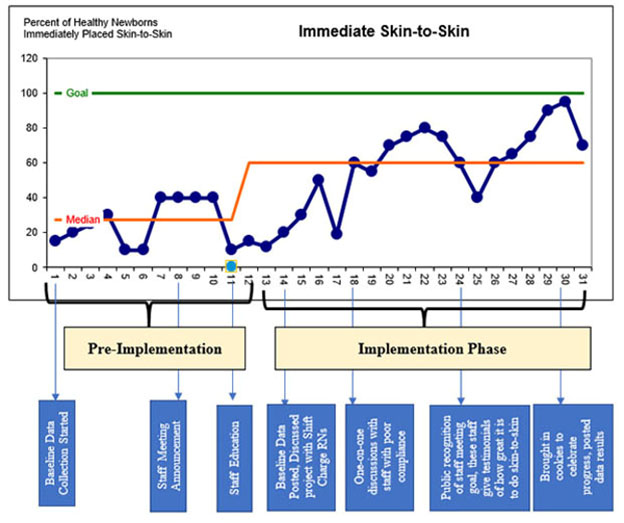
Example of a Run Chart
Figure 1 is an example of a run chart that tracked the percent of healthy newborns toward the goal of being placed skin-to-skin immediately after birth during the month of March. Analysis of this run chart data would suggest that there was an increasing trend in the percentage of newborns who were placed skin to skin over the 31days that the initiative was being tracked.
This website is maintained by the University of Maryland School of Nursing (UMSON) Office of Learning Technologies. The UMSON logo and all other contents of this website are the sole property of UMSON and may not be used for any purpose without prior written consent. Links to other websites do not constitute or imply an endorsement of those sites, their content, or their products and services. Please send comments, corrections, and link improvements to nrsonline@umaryland.edu.